Bringing research back to the Emergency Department
An interview with Rebecca Miln, Senior Research Nurse, Division 6, Poole Hospital, University Hospitals Dorset NHS Foundation Trust.
When I began my career as a nurse, I worked in the Emergency Department (ED) for six years then went into haematology and oncology, then oncology research.
When I side-stepped into oncology research, I really enjoyed the exposure I had to research but over time I missed acute medicine – emergency care and acute treatment has always been my passion. During the pandemic, I had the opportunity to step up as a Senior Research Nurse and was involved in public health research with the RECOVERY trial, which gave me the opportunity to blend research with acute treatment.
I was on the lookout for other studies and approached the NIHR, who were funding the PRONTO trial and put it on my radar. The EDs at Poole and Royal Bournemouth Hospital hadn’t run research for a number of years, so I knew it would be a challenge to get the study up and running because EDs are always so busy. However, I have a good relationship with the consultant there and he was interested in the study, so we decided to give it a go.
The Pronto Study
Currently in ED, we use a tool called the NEWS2 score to aid early recognition of seriously unwell patients. Those who have a high NEWS2 score could be at greater risk of sepsis but it’s important to know that you can have a high NEWS2 score for multiple reasons, it doesn't always suggest a patient has sepsis. In some people it can be perfectly normal to have a high NEWS2 score. What we worry about is either missing sepsis or overtreating when it’s not necessary. Further down the line, when the blood results have been analysed, you find there are a lot of patients that aren’t actually septic. If we continue to overtreat, are people going to be resistant to broad-spectrum antibiotics in ten years’ time? It also costs the trust a lot of money, so if we can more accurately diagnose and treat sepsis then it helps everyone.
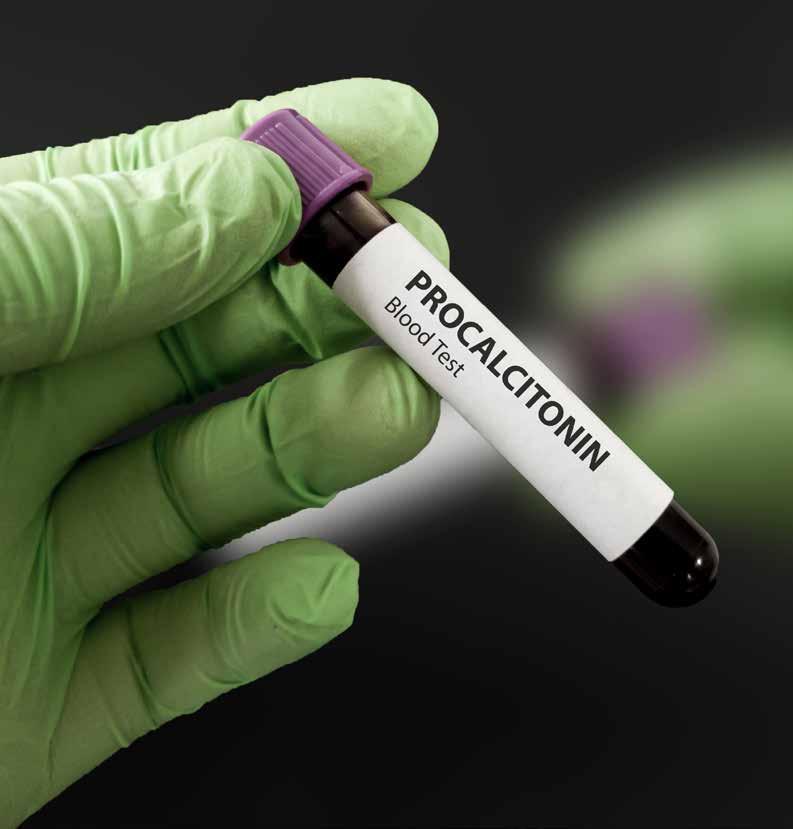
The PRONTO study uses a blood test called PROcalcitonin which gives us a much clearer indication of bacterial infection. The result combined with the NEWS2 score provides more information to support clinicians to treat appropriately early on in the patient’s journey.
From the moment we think a patient might have sepsis, we enrol them into the study. We first randomise them via an iPad, which selects which arm of the trial they go into. For patients selected to receive the PROcalcitonin test, we take a blood sample and get the results in 20 minutes. With the NEWS2 score alone, we can’t tell if there is a viral or bacterial infection, or something else, it’s just numbers.
Because of the nature of sepsis and the need to diagnose and treat quickly, we use a deferred consent process. When I’m with the patient, I talk them through what we’re doing and why but as you can imagine, these patients are quite unwell and unable to take in lots of information. Most patients who have then been diagnosed with sepsis have been so grateful to have had the test and be part of the research.
PRONTO opened at Royal Bournemouth Hospital in April 2021 and currently has over 100 participants enrolled into the study. In Poole, we have recruited more than 50 participants since the study opened in July 2022. PRONTO is due to end around May 2023, with the results expected shortly after.

Getting Engagement
Getting engagement from busy EDs can be difficult. When I taught initially at the hospital to establish the study, I made it really clear that there would be no additional workload for the emergency care teams. The trial team would be there to assess patients, randomise and carry out any related tasks.
It took about six months to set up the study and get it ready to accept patients. The first two months of the study being open were tricky and I needed to be very present which was a challenge at times. It was important for me to be available to answer any questions that helped people to engage and understand, and for me to teach during quiet moments. I’ve had to wear a lot of hats!
I am really lucky to have engaged Principal Investigators (PI) at Bournemouth and Poole, who do a wonderful job at raising the profile of the study and disseminating information about it. It wouldn’t have been as successful without them.
The engagement has been amazing since opening. People were so keen to be involved and asked for extra training sessions to know more. The staff now get in touch with the research team if they have any patients who may be eligible which is fantastic and a positive step forward for embedding research in ED.
Challenging the Status-Quo
Of course, the trial has huge benefits for our patients. But what we're also doing is raising awareness of research and inspiring staff to get involved. We're showing that even in a busy department, there is still time for research and research active hospitals are generally safer and deliver better care.
It's important to share the motivation for the trial – this could be something that shapes the future of emergency care and how we diagnose and treat sepsis. Not only does the work we’re doing help guide potential diagnoses, but it also helps to refresh people’s knowledge on sepsis. The guidelines change all the time so it keeps people up-to-date.
Research is really on the map because of the pandemic and PRONTO is part of the NIHR’s Associate PI scheme, which helps to embed research within clinical settings by providing practical experience for healthcare professionals starting their research career. I think previously, people assumed that research nurses sat at desks and wrote up lots of reports on trials – but now they can see that we’re incredibly patient-facing. We’re able to offer patients treatments and investigations that they wouldn’t normally have access to, which can help to deliver better care.
After the study was established at both hospitals, I was invited to give a talk to advanced nurse practitioners. It was fantastic that they had thought about research – they were so engaged. Someone at that talk now works at Poole Hospital and wants to be involved with research.
I really hope that the results of the PRONTO trial show a positive impact and that we could potentially influence standard emergency care across the country. That’s a really exciting prospect.
I hope that people will begin to approach us to see what else we can do and change. Even if the outcome is that it doesn’t work, we still need to know that – it’s important to know what doesn’t work just as much as what does work.