‘Pill on a string’ test can ‘transform oesophageal cancer diagnosis’
A ‘pill on a string’ test can identify ten times more people with possible early signs of oesophageal cancer than the usual GP route, NIHR-supported research found.
The test can diagnose more with Barrett’s oesophagus, a condition that can lead to oesophageal cancer in a small number of people, research published in The Lancet found.
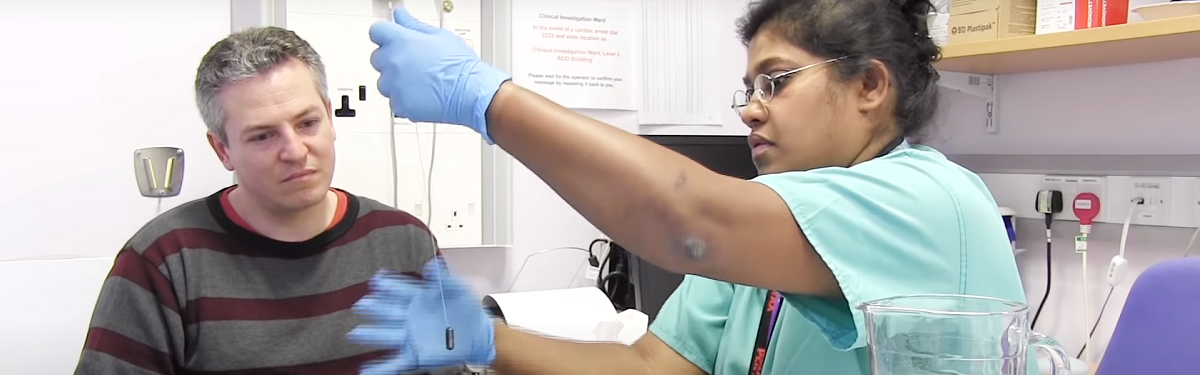
The Cytosponge test involves a small pill with a thread attached that the patient swallows and expands into a small sponge when it reaches the stomach.
This is quickly pulled back up the throat by a nurse, collecting cells from the oesophagus for analysis.
The test, which can be carried out by a nurse in a GP surgery, is also better at picking up abnormal cells and potentially early-stage cancer.
Barrett’s oesophagus is usually diagnosed in hospital by endoscopy – passing a camera down into the stomach – following a GP referral for long-standing heartburn symptoms. It is hoped the test will help doctors better identify which patients will need an endoscopy.
About 9,200 people are diagnosed with oesophageal cancer in the UK each year and about 7,900 die. Some 85% with the earliest stage
in England survive for a year or more compared to 21% if diagnosed at the most advanced stage.
The Cancer Research UK-funded study involved 13,222 participants randomly allocated the sponge test or standard care, including 1,318 in nine Oxfordshire GP practices.
Over a year, the odds of detecting Barrett’s were ten times higher in those offered the Cytosponge with 140 cases diagnosed compared to 13 in usual care.
The Cytosponge also diagnosed five cases of early cancer (stage 1 and 2), whereas only one case of early cancer was detected in the GP group.
Alongside better detection, the test means cancer patients can benefit from less severe treatment if it is caught at an earlier stage.
The University of Cambridge’s Professor Rebecca Fitzgerald, who led the research, said: “It’s taken almost a decade of research and testing thousands of patients to show that we’ve developed a better route to diagnosing Barrett’s oesophagus.
“And the sponge could also be a game-changer in how we diagnose and ensure more people survive oesophageal cancer. Compared with endoscopies performed in hospital, the Cytosponge causes minimal discomfort and is a quick, simple test that can be done by a GP.
“Our test is already being piloted around the country, so we hope more people across the UK could benefit from it.”
The researchers are putting the test through an economic evaluation and hope it will be rolled out to GP practices within three to five years.



